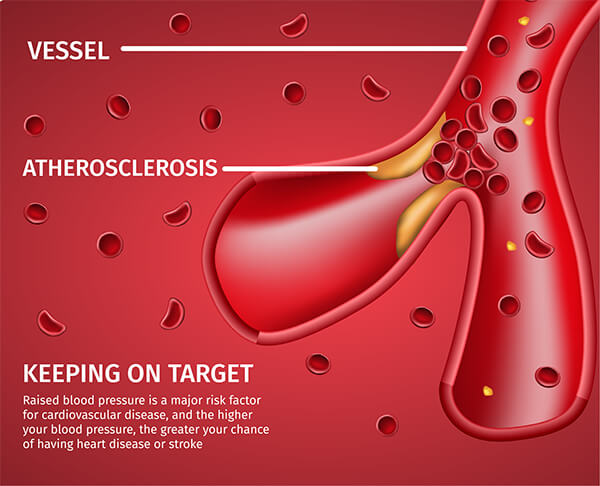
PERIPHERAL ARTERIAL DISEASE (PAD) IS A COMMON CIRCULATORY PROBLEM. THE ARTERIES THAT CARRY BLOOD TO YOUR HEAD, ORGANS, AND LIMBS BECOME NARROWED BY THE BUILDUP OF ARTERIAL PLAQUE (ATHEROSCLEROSIS), REDUCING BLOOD FLOW.
Symptoms of neuropathy including burning, tingling, numbness and pain can also be a sign of PAD—which left untreated can become life threatening. Many who have been told they have neuropathy find that medication, surgery, or other treatments simply aren’t working—and that’s when they turn to us for help. We welcome you to use this website as a resource to learn more about PAD and please feel free to contact us to learn about treatment for PAD without the need for invasive surgery. Most insurance and Medicare accepted.
Eight million Americans
suffer from PAD
PAD affects 20% of
patients over age 75
One in three diabetics
over age 50 suffer from PAD
Smoking increases the
likelihood of developing
PAD by 400%
Each year, approximately
150,000 lower-limb
amputations in the U.S. can be attributed to PAD
About 20-25% of people
with PAD are asymptomatic
and don’t know they have it.
WHAT IS PAD
What is Peripheral Artery Disease (PAD)?
Your arteries are the vessels in the circulatory system which deliver oxygen-rich blood from your heart to the rest your body. Peripheral artery disease (PAD) is a narrowing of the arteries that happens when fatty plaque builds up and hardens along the walls. This hardened plaque reduces the amount of blood that is able to flow through the arteries. When there is not enough blood flow, it causes pain. This type of pain is called claudication. It usually happens in the legs when you exercise or walk. It is often an indication of PAD. The pain often subsides when you rest, but as the disease progresses it can cause leg pain at any time.
It’s tempting to blame your aching legs on normal aging but left undiagnosed and untreated PAD can seriously impact your mobility and reduce your quality of life. Lack of circulation in the feet, ankles and legs can lead to non-healing wounds, gangrene, and possible amputation. The narrowing of your arteries isn’t limited to your lower body, either. People with PAD are also at higher risk for stroke and heart attack.
Diagnosing PAD is simple and easy on the patient. There is no reason not to seek answers for this condition. The sooner you seek help, the better the impact will be on your overall health, mobility, and quality of life.
A Race Against Time
A Race Against Time
PAD doesn’t happen overnight; it happens over time. And like all things that happen over a span of time you may consider physical change to just be a part of getting older. One of the biggest concerns surrounding peripheral artery disease (PAD) is waiting to seek treatment while the symptoms progress. PAD can sneak up on you. You may be ignoring the telltale signs of the condition because you think it’s a natural part of getting older.
PAD can start with a pain in your calf when you walk, but it goes away when you take a break. As the condition progresses, you may experience pain or cramps in your legs at night when you’re laying down. But, standing up relieves that pain, so you rationalize it because it has passed. Numbness, burning pain, or tingling in your feet are also signs to pay attention to.
If you have difficulty walking without taking a break, your feet feel numb, or your legs cramp in bed at night, you should start asking questions. It may be due to poor circulation. Your circulatory system carries blood throughout your body. That blood supplies oxygen and nutrients to your nerves and tissues. When that supply is reduced, you start developing symptoms of PAD. If it goes untreated, serious consequences will follow.
People who suffer from PAD have an increased risk for developing coronary artery disease and cerebrovascular disease, which can lead to heart attack and stroke. Visiting your doctor at the first sign of any of the symptoms makes a difference. The sooner you identify the condition, the better it is to manage it and lower your risk for complications.
There are certain factors which put people at higher risk for developing PAD. Some you can’t control like aging, family history of PAD, heart disease or stroke. But others you can, like smoking, obesity, inactivity, high blood pressure, high cholesterol, and diabetes. If any of these conditions apply to you, you and your doctor should be on the lookout for PAD.
LOWERING YOUR RISKS
Quitting Smoking
Losing Weight
Increasing Activity
Managing High Blood Pressure & Cholesterol
Managing Diabetes
Peripheral Arterial Disease (PAD)
SYMPTOMS
My legs hurt. Could it be PAD?
Leg cramps or pain when walking, cold feet or legs, pain in your legs even when resting, sores that don’t heal, are all indicators for PAD. If you are experiencing any of these symptoms, talk with your primary care doctor or specialist. However, some people with PAD don’t notice any symptoms at all. This is why communication and watchfulness are a vital part of maintaining good health.
The most common symptoms include:
Muscle Cramping – Intermittent Claudication. Pain while exercising is called claudication. Itis the most common symptom of PAD. Some people experience a dull ache or heaviness in the legs rather than outright pain. You may have a hard time walking or climbing stairs without having to stop and rest.
Abnormal pulse. The pulse in the legs may be reduced or even absent if you have PAD.
Temperature changes. If one foot is noticeably colder than the other, it could be due to PAD.
Pain at rest. More severe cases of PAD can cause pain in the legs even at rest. The discomfort may keep you up at night.
Non-healing wounds. Sores or wounds on the toes, feet or ankles that are not healing may be a sign of PAD.
Maybe it’s Not Neuropathy
Neuropathy is a condition that involves damage to the peripheral nervous system. Muscle cramping, difficulty walking, burning, tingling, numbness, and pain in the legs and/or feet are symptoms people living with neuropathy experience on a daily basis. These symptoms are very similar to those of PAD. They are so similar that in many cases, people are given a diagnosis of neuropathy when in reality it isn’t.
Unfortunately, there is no cure for neuropathy. Medications suppress the symptoms and trick the body into not noticing them. However, if you don’t have neuropathy, you are masking the problem and allowing the real cause (in many cases PAD) to get worse.
It’s important to get to the root of the problem and oftentimes it’s poor circulation. So, if you’ve been told you have neuropathy, and you’re not finding relief from medication or treatment, consider the fact that it might not be neuropathy. It could be PAD that’s causing your pain and impacting your everyday living. And the good news is, there are treatments for PAD.
next steps
Diagnosing PAD
What should I do if I suspect I have PAD?
If you suspect you may have PAD, it is critical to get a diagnosis and begin treatment and lifestyle changes as soon as possible. Proper care can slow the disease or stop it from progressing.
Most diagnostic procedures for PAD are easy and painless. Your doctor may conduct one or more of the following tests to confirm a diagnosis of PAD.
- Ankle-brachial index (ABI). Your doctor will take the blood pressure in your arm and compare it to the blood pressure in your ankle. This may be done at rest and also while you are walking on a treadmill to determine how exercise affects blood flow.
- Transcutaneous pulse oximetry. This non-invasive test involves placing electrodes on the skin to measure oxygen levels in the tissue below.
- Duplex Ultrasound. Non-invasive Doppler ultrasound can show how well blood is flowing through your blood vessels and identify any narrowing or blockages.
- Dye is injected into your vascular system and blood flow is evaluated using computerized tomography (CT) or magnetic resonance (MR) visualization.
- Blood test. An analysis of your blood can reveal your levels of cholesterol, triglycerides, and blood sugar.
treatment
So, I have PAD. Now what?
PAD is a serious disease, but it is treatable. If you are diagnosed with PAD, your treatment will have two goals:
- Reduce and manage leg pain so that you are able to exercise
- Stop additional plaque buildup to lower your risk of stroke, heart attack and symptom progression
If your PAD has progressed, your doctor may refer you to an endovascular specialist for a minimally invasive, in-office procedure to open your arteries and improve blood flow.
Lifestyle changes. In the early stages of PAD, treatment might involve only lifestyle changes. If you smoke, the single most important thing you can do to stop PAD from progressing is to quit. Your doctor will also recommend a diet and exercise regimen to improve your circulatory health.
Medication. Your doctor may prescribe medications to lower your blood pressure and cholesterol, manage blood sugar levels, and/or improve blood flow.
Angioplasty/Stenting. This procedure uses a balloon to widen narrowed arteries. A small wire cage called a stent may be placed in the blood vessel to keep it open.
Atherectomy. This procedure uses special tools to clean plaque out of affected arteries. Minimally invasive techniques are used, making this procedure easy on the patient with little downtime or pain.
Bypass grafting. During this surgical procedure, doctors create a clear path for blood to flow past the blocked arteries.
clock is ticking
What if I don’t do anything?
PAD is a serious disease that requires treatment and management. Symptoms may happen in your legs and feet, but plaque buildup is happening throughout your body.
Ignoring PAD can lead to serious consequences. Left untreated, patients with PAD can eventually suffer from:
Critical Limb Ischemia (CLI). When PAD becomes advanced, blockages to the lower extremities can be so severe that they cause extreme pain in the feet or toes, numbness, non-healing wounds, and even infections or gangrene. Over time people with CLI may not be able to walk at all. Wounds that won’t heal may lead to amputation. If you have an amputation due to PAD your life expectancy is worse than if you had breast cancer or lymphoma.
Heart Attack, Stroke, or transient ischemic attack (TIA). Symptoms of PAD can be an indication that blood flow to major organs is reduced as well. A heart attack occurs when the heart muscle does not receive adequate blood flow. A stroke occurs when the blood supply to the brain is interrupted or reduced. A TIA is a very temporary interruption of blood flow to the brain.
Renal Artery Stenosis. PAD is associated with renal artery stenosis. Blockages in the arteries that feed the kidneys can lead to fluid retention in the legs, high blood pressure, fluid buildup in the lungs and kidney failure.